Media for Staphylococcus Aureus Detection
Staphylococcus aureus is frequently a part of our skin flora but is also a cause of a broad range of illnesses. Current studies report a remarkable increase of Methicillin Resistant Staphylococcus aureus (MRSA) over recent years.
Staphylococci may be airborne and can occur in both animals and humans, in sewage, water, milk or food, and on environmental surfaces or food equipment. It is still one of the five most common causes of nosocomial infections, often causing postsurgical wound infections. Consequently, it poses a major concern in hospitals, especially in regard to MRSA, methicillin-resistant Staphylococcus aureus.
Staphylococcus aureus is an invasive pathogen that can cause disease in almost any tissue or organ in the human body, primarily in compromised individuals. Staphylococcal infections were treated using penicillin, but over the years this pathogen developed resistance to penicillin by building penicillinase. Methicillin was the next drug of choice as it is not cleaved by the penicillinase. While methicillin is very eff ective in treating most Staphylococcus infections, some strains have developed resistance to methicillin by production of penicillin-binding protein, and can no longer be killed by this antibiotic. These resistant bacteria are called Methicillin Resistant Staphylococcus aureus (MRSA)1. Patients with breaks in their skin due to wounds, indwelling catheters or burns are at high risk of developing MRSA infection 2. Spread of MRSA infections can be controlled to a great extent by maintaining personal hygiene after interaction with an MRSA-infected person1.
Today there are many innovative solutions to detect MRSA. We strongly support the microbiologist with a selective chromogenic HiCrome MeReSa Agar for detection of MRSA from clinical isolates and other samples. The proprietary chromogenic mixture incorporated in the medium is specifi cally cleaved by S. aureus to give bluish-green colonies on this medium and can be clearly diff erentiated from other species. The medium is made selective for MRSA by the addition of methicillin.
Product Listings

Foods that are frequently associated with staphylococcal food poisoning include meat and egg products, milk and dairy products, and various other products that may contain these food ingredients. Processes in the food industry that are kept at slightly elevated temperatures must guard against staphylococcal food poisoning, one of the leading causes of gastroenteritis. The food poisoning is due to the presence of staphylococcal enterotoxins produced by Staphylococcus aureus in the food.
Staphylococci are facultative anaerobes Gram-positive bacteria that grow by aerobic respiration or by fermentation that yields principally lactic acid. The bacteria are catalase-positive and oxidase-negative. S. aureus produce diverse enzymes such as staphylokinase (coagulase), proteases, phopshatase, a lipase, a deoxyribonuclease (DNase) and a fatty acid modifying enzyme (FAME). The majority of clinical isolates of S. aureus express special surface polysaccharide and protein A. Diff erentiation and identifi cation of S. aureus can be made based on these biochemical characteristics. More details may be found in the ID flow chart (Figure 2), the table of kits and tests (Table 1), and the table listing media for the differentiation of Staphylococcus aureus (Table 2).
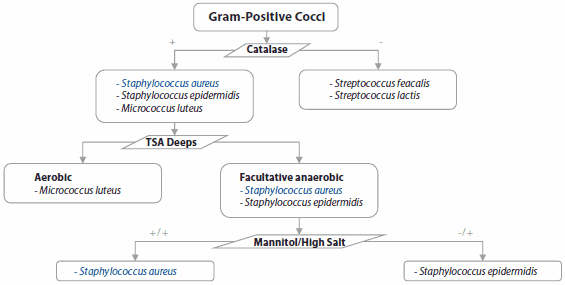
Figure 2.ID flow chart for Staphylococus aureus
Table 1 and Table 2 specify characteristics which kits and tests utilise for the identification of S. aureus.
References
To continue reading please sign in or create an account.
Don't Have An Account?